What is Diabetic Retinopathy?
Approximately half of all diabetics will develop diabetic retinopathy. Patients with diabetes mellitus (DM) can have abnormal blood sugar levels which can damage normal blood circulation throughout the body, including the eye.In diabetic retinopathy (DR), high blood sugar levels cause damage to blood vessels in the retina which can impact vision.
There are three main ways that diabetic retinopathy causes vision loss:
- Diabetic macular edema (DME) — fluid build-up in the central portion of the retina
- Proliferative diabetic retinopathy (PDR) — growth of abnormal blood vessels into and on top of the retina
- Iscchemia — retinal cell death or dysfunction due to lack of oxygen in the retinal tissue
Diabetic retinopathy can affect type I (insulin dependent) and type II (non-insulin dependent) diabetics. The board-certified retina specialists at Retina Consultants of Texas are trained to diagnose diabetic retinopathy and help patients manage the condition.
Dr. Brown: Diabetic Retinopathy
Types and Stages of Diabetic Retinopathy
There are two main types of diabetic retinopathy: non-proliferative and proliferative.
Non-proliferative Diabetic Retinopathy (NPDR): Non-proliferative diabetic retinopathy (NPDR) and background diabetic retinopathy (BDR) describe early stages of diabetic retinopathy. Blood vessel damage in diabetic retinopathy can lead to abnormal leakage of fluid and blood into the retina. This leakage can cause the retina to swell. If this swelling occurs in the macula, it is called diabetic macular edema (DME), and vision can be affected. This is the most common cause of visual loss in patients with diabetes and ranges from mild to severe.
Proliferative Diabetic Retinopathy (PDR): PDR occurs when abnormal blood vessels grow into and on top of the retina. These abnormal blood vessels are fragile and can bleed into the eye causing vitreous hemorrhage. This can cause dark floaters and may cause immediate and severe loss of vision. Pulling and contraction of these abnormal vessels and their associated scar tissue on the retina can lead to a tractional retinal detachment, a condition where the retina is pulled away from the back of the eye leading to loss of vision.
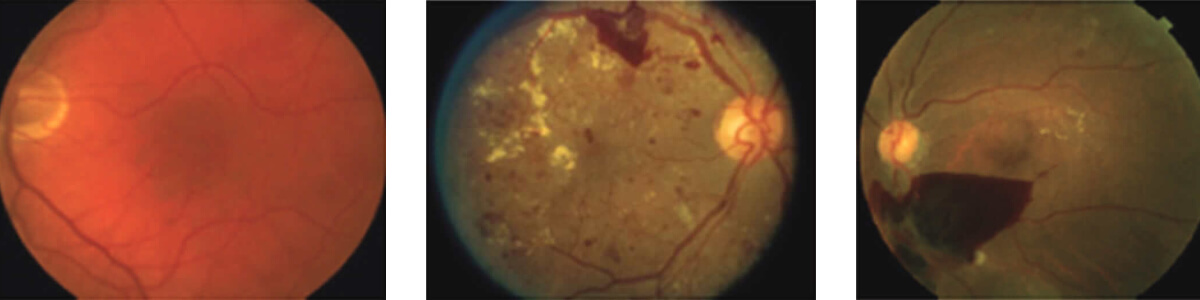
From left to right: Normal macula, Diabetic Macular Edema (DME), Proliferative Diabetic Retinopathy (PDR)
Causes and Symptoms of Diabetic Retinopathy
In its earliest stages, diabetic retinopathy typically has no symptoms. That is why it is important for patients with diabetes to take a preventive approach. All diabetics should see their ophthalmologist for a comprehensive dilated fundus eye exam at least once a year. In addition, it is important to control blood sugar, blood pressure and cholesterol levels. Early detection of diabetic retinopathy allows the best chance for maintaining good vision.
As diabetic retinopathy progresses, common symptoms patients may experience include:
- Blurry or distorted vision
- A decrease in visual acuity (sharpness)
- Floaters
- Muted color detection
- Vision loss
Diagnosis
Diabetic retinopathy is diagnosed by your ophthalmologist during a dilated eye exam. Your doctor may obtain photographs of the retina and diagnostic tests, including ocular coherence tomography(OCT) and fluorescein angiography (FA), to help guide treatment. With OCT, light waves are used to capture detailed images of the retina. With FA, a special dye is injected into your bloodstream through an IV. This highlights the blood vessels in the retina so we can determine if there is any bleeding, leakage, or damage.
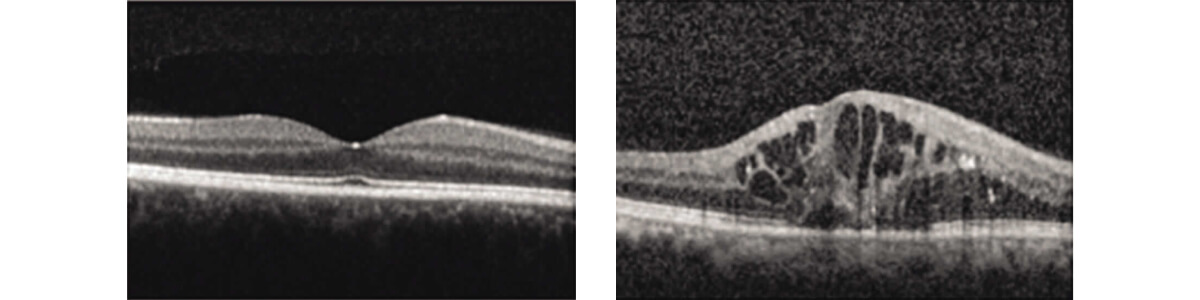
Left: Normal macula OCT, Right: OCT of severe DME with retinal thickening, cysts, and subretinal fluid
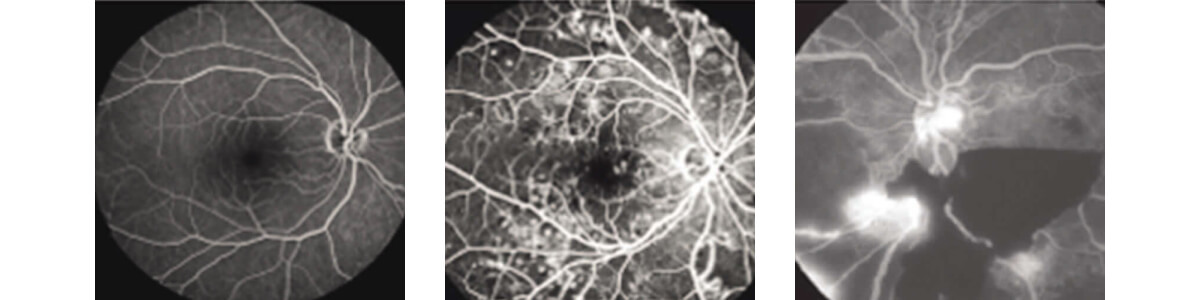
From left to right: Normal FA, DR with widespread blood vessel damage, PDR with leaking abnormal blood vessels and blood in front of retina
Treatment and Prognosis
Prevention is the best treatment for diabetic retinopathy. Optimal blood sugar, blood pressure, cholesterol and weight control can reduce the long-term risk of vision loss from diabetic retinopathy. Cooperation with your primary care physician is very important to help keep your diabetes and other cardiovascular risk factors under control.
Once the diagnosis of diabetic retinopathy has been made, you may require more frequent eye exams. In addition, checking your blood sugar at home, recording your blood sugars in a notebook, and showing these numbers to your primary care physician are critical to success in controlling your disease.
Medical Treatment
Medical treatment for diabetic retinopathy may involve the use of injections of medicine into your eye (intravitreal injections) to treat the build up of fluid (diabetic macular edema). Recent science has shown that DME and PDR are controlled by a signal sent from the damaged retina called vascular endothelial growth factor (VEGF). Several VEGF blocking drugs (including Lucentis, Avastin and Eylea) and other medications (steroids and steroid implants) when injected into the eye can cause DME and PDR to regress. Most of these agents provide only temporary relief and need to be given repeatedly over a prolonged period of time.
Laser Treatment
Laser treatment may be recommended for people with diabetic macular edema (DME). The goal of this treatment is to prevent further vision loss. The laser seals leaking blood vessels, reduces swelling and prevents new abnormal blood vessels from growing. For macular edema, the laser is focused on parts of the retina outside of the macula. Multiple laser treatments may be necessary. Laser treatment is not a curative procedure and does not always prevent further loss of vision.
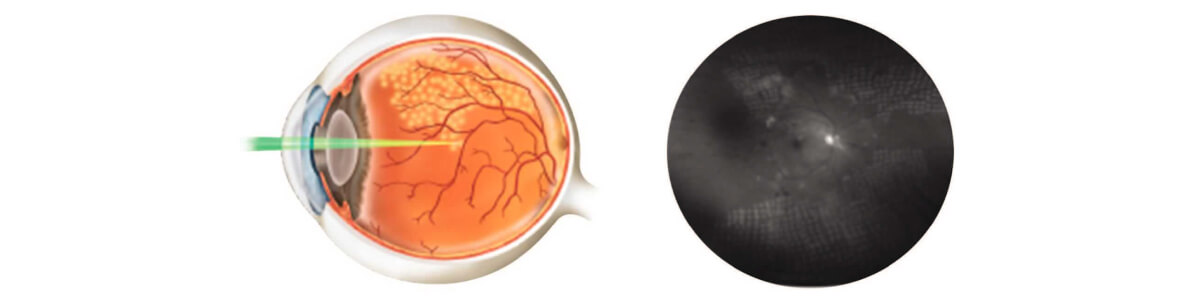
Left: Schematic of how retinal laser spots are applied; Right: PRP (Panretinal Photocoagulation) spots immediately following laser surgery for PDR
Surgical Treatments
Vitrectomy surgery in the operating room may be recommended if bleeding from diabetic retinopathy causes a vitreous hemorrhage and associated vision loss. Additionally, surgery may be needed to treat tractional retinal detachment in the setting of extensive blood vessel and scar tissue growth.
Vitrectomy surgery requires a team approach. Before surgery, you will likely need to have a physical examination with your general doctor to identify and possibly treat any medical conditions. Your surgeon and anesthesiology team will decide whether local or general anesthesia is appropriate for you. Most vitrectomy surgeries are performed as outpatient procedures with local anesthesia, and the patient may go home the same day. The length of the operation varies from 20 minutes to several hours depending on your condition. Other procedures may be combined with your vitrectomy, including peeling membranes or laser application, depending on your specific needs. Your surgeon will perform your vitrectomy using a microscope and tiny instruments that are placed into your eye through small incisions in the sclera, the white part of your eye.
If you have any questions or concerns about treatment, please discuss them with your diabetic retinopathy specialist at Retina Consultants of Texas.
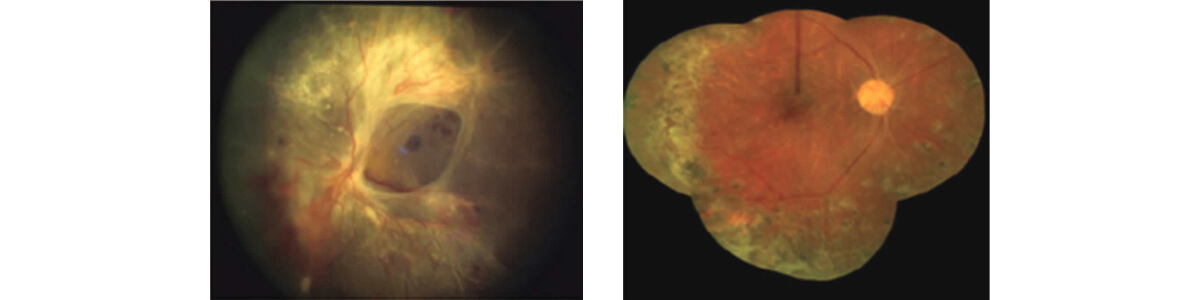
Left: Pre-operative photo of a patient with a sever tractional retinal detachment; Right: Post-operative photo of a patient following successful vitrectomy surgery
Learn More About Diabetic Retinopathy
Visit Retina Consultants of Texas for Diabetic Retinopathy Treatment in Houston and San Antonio
At Retina Consultants of Texas, preserving your vision is our mission. We offer a full spectrum of retinal care using the most advanced technologies to address diseases of the retina, macula, and vitreous. For world-class retinal care, including diabetic retinopathy treatment, schedule an appointment with RCTX in the Greater Houston and Greater San Antonio, TX areas today.



